
Stroke Causes, Symptoms, and Recovery
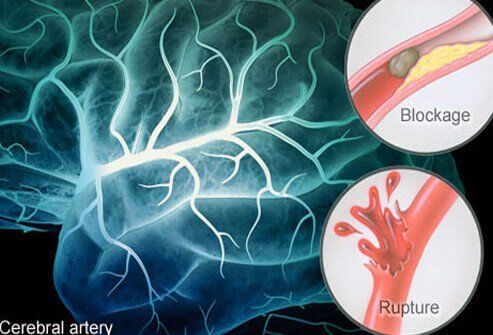
When the brain's blood supply is inadequate, a stroke results. Stroke symptoms (for example, loss of arm or leg function or slurred speech) signify a medical emergency because without treatment, blood-deprived brain cells quickly become damaged or die, resulting in brain injury, serious disability, or death. Call 9-1-1 if you notice stroke symptoms developing in someone.
Stroke Symptoms
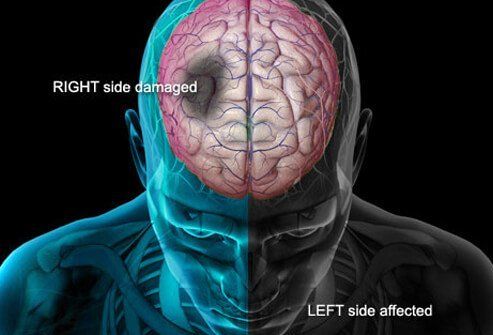
Initial symptoms of a stroke can occur in someone suddenly. Know these signs of a stroke:
Difficulty speaking
Difficulty understanding or confusion, especially with simple tasks
Difficulty with muscle strength, especially on one side of the body
Numbness, especially on one side of the body
Severe headache
Vision changes (in one or both eyes)
Difficulty with swallowing
Facial droop on one side
Signs of a Stroke

The F.A.S.T. test was designed in 1998 to help ambulance staff in the United Kingdom quickly assess stroke. It takes into account the most common symptoms of stroke and is designed to help quickly assess a stroke with very little training.
F.A.S.T. Test
F means face: If one side of the face droops, it’s a sign of a possible stroke
A means arms: If the person cannot hold both arms out, it’s another possible stroke sign
S means speech: Slurring words and poor understanding of simple sentences is another possible stroke sign
T means time: If any of the FAS signs are positive, it’s Time to call 9-1-1 immediately
Strokes and the Brain
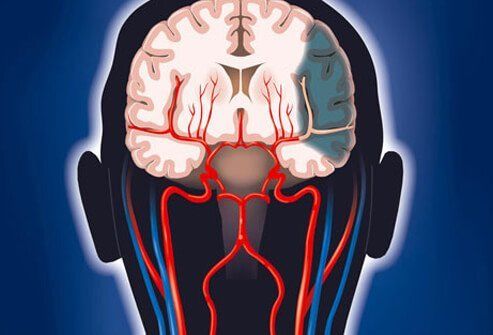
Remember the FAST test for stroke. The “T” in FAST also means the longer the brain is blocked from its blood supply (usually due to a blood clot), the greater the brain damage possible.
For many patients, the time limit to diagnose and treat such a clot is usually within 3 hours (some physicians suggest a bit longer). In some qualified patients, the use of a clot-busting drug may be used to dissolve the clot and restore blood flow. Not all patients qualify for this treatment. There are also some risks like bleeding associated with this treatment that may cause problems.
Strokes are a leading cause of long-term disability in people.
Diagnosing Types of Strokes

There are two main types of strokes (ischemic and hemorrhagic) and they are treated differently. They are often emergently diagnosed by a head CT scan (or an MRI scan).
Ischemic Stroke
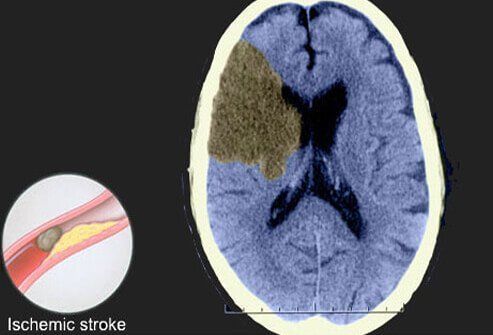
This slide shows a CT scan of an ischemic stroke, which is responsible for about 80% to 90% of all strokes. Ischemic strokes are caused by clots that reduce or stop blood flow to the brain. The clot may develop elsewhere in the body and circulate to become lodged in a blood vessel in the brain, or the clot may originate in the brain.
Ischemic strokes are usually divided into two main subtypes: thrombotic and embolic.
Thrombotic Stroke
Nearly half of all strokes are thrombotic strokes. Thrombotic strokes are caused when blood clots form in the brain due to a diseased or damaged cerebral artery.
Embolic Stroke
Blood clots also cause embolic strokes. However, in the case of embolic strokes, the blood clot forms in an artery outside the brain. Often these blood clots start in the heart and travel until they become lodged in an artery of the brain. The physical and neurological damage embolic strokes cause is nearly immediate.
Hemorrhagic Stroke
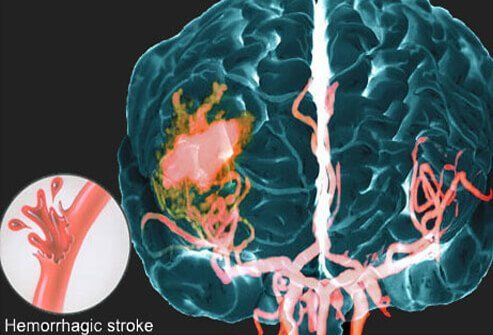
This picture shows a hemorrhagic stroke using an MRI image. The circle inset outlines what composes a hemorrhagic stroke. A blood vessel in the brain breaks open, and blood escapes into the brain under pressure, compressing other blood vessels and brain cells causing damage and death. This bleeding into the brain is difficult to stop and is more likely to be fatal. There are two types of hemorrhagic strokes: intracerebral and subarachnoid.
Intracerebral Stroke
“Intracerebral” means “within the brain,” and it refers to a stroke caused by a diseased blood vessel bursting within the brain. Intracerebral strokes are usually caused by high blood pressure.
Subarachnoid Stroke
A subarachnoid hemorrhage refers to bleeding immediately surrounding the brain in the area of the head called the subarachnoid space. The main symptom of a subarachnoid stroke is a sudden, severe headache, possibly following a popping or snapping feeling. Many factors can cause a subarachnoid stroke, including head injury, blood thinners, bleeding disorders and bleeding from a tangle of blood vessels known as an arteriovenous malformation.
Mini-Stroke (TIA)
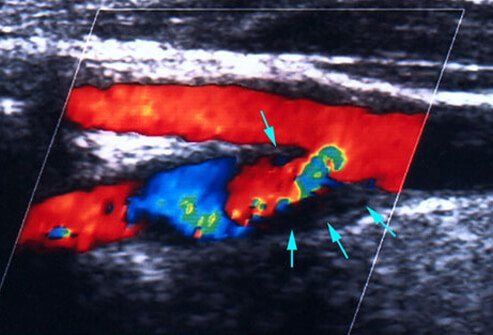
"Mini-strokes" (also termed transient ischemic attacks or TIAs) are temporary blockages of blood vessels in the brain. TIAs can produce mild stroke symptoms that resolve. TIAs often occur before a stroke happens, so they serve as warning signs that the person may need stroke preventive therapy.
Mini Stroke Symptoms
Confusion
Weakness
Lethargy
Paralysis
Facial droop
Vision loss
Mini Stroke Treatment
Treatment for a mini-stroke may include medication, changes in lifestyle, and possibly surgery to reduce the chances of another stroke occurring.
What Causes a Stroke?
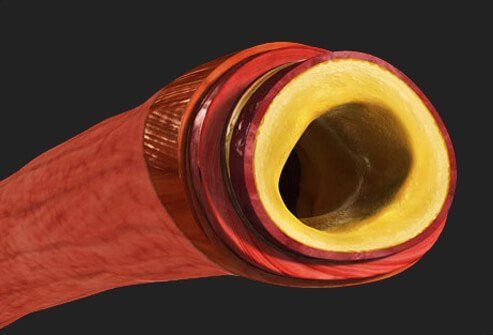
Common causes of stroke come from blood vessels both outside and inside the brain. Atherosclerosis (hardening of the arteries) can occur when plaque (deposits of cholesterol, calcium, fat, and other substances) builds up and narrows the vessel, making it easy for clots to form and further occlude the vessel. The clots can break free only to travel to and block smaller vessels inside the brain. The blood vessels inside the brain itself can accumulate this plaque. Occasionally, weakened vessels can burst and bleed into the brain.
Stroke Prevention: Managing Medical Conditions

Common conditions that increase a person's risk for strokes include high blood pressure, elevated cholesterol levels, diabetes, and obesity. People can reduce stroke risks by addressing these problems.
Lifestyle Changes

People can also reduce their stroke risk by altering some aspects of their lifestyle. For example, people who stop smoking, begin a consistent exercise program, and limit their alcohol intake (two drinks per day for men, one per day for women) can decrease their risk.
Stroke Prevention: Diet

One of the best ways to reduce stroke risk is to eat a diet that has low fat and low cholesterol to reduce the chance of plaque formation in blood vessels. Foods high in salt may increase blood pressure. Cutting back on calories can help reduce obesity. A diet that contains a lot of vegetables, fruits, and whole grains, along with more fish and less meat (especially red meat) is suggested to lower stroke risk.
Uncontrollable Stroke Risk Factors

Unfortunately, there are some risk factors that people cannot control, such as family history of strokes, gender (men are more likely to have a stroke), and race (African Americans, Native Americans, and Alaskan Natives all have increased risk for strokes). In addition, women who get strokes are more likely to die from the stroke than men.
Emergency Stroke Treatment
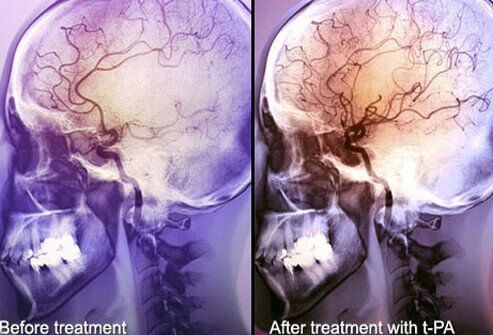
Emergency stroke treatment depends on the type of stroke and underlying health of the patient. Ischemic strokes are treated by methods designed to remove (dissolve) or bypass a clot in the brain, while hemorrhagic strokes are treated by attempts to stop the bleeding in the brain, control high blood pressure, and reduce brain swelling. Hemorrhagic strokes are more difficult to treat.
Aspirin
Aspirin is part of a group of drugs called antiplatelet agents. Antiplatelet agents like aspirin help prevent blood cell fragments from sticking together and forming clots and are therefore helpful in preventing some forms of stroke. The American Heart Association recommends taking aspirin within two days of an ischemic stroke to reduce the stroke’s severity. For those who have had a mini-stroke, a doctor may recommend daily aspirin treatment.
TPA
TPA is a clot-busting drug that can be used to treat ischemic strokes. It is given through the arm as an IV and helps dissolve blood clots and improve blood flow through areas of the brain blocked by clots. TPA may help if it is used within three hours of a stroke taking place.
Stroke Recovery

Strokes that cause long-term damage are usually severe and/or not treated or treated after large sections of the brain have been damaged or killed. The type of damage depends on the location in the brain where the stroke occurred (for example, the motor cortex for movement problems or the brain area that controls speech). Although some problems will be permanent, many people that do rehabilitation can regain some or many of the abilities lost in the stroke.
Speech Therapy

If a stroke damages a person's ability to use language and to speak or swallow, rehabilitation with a speech therapist can help a person regain some or most of the abilities they lost initially with the stroke. For those who have severe damage, rehabilitation can provide methods and skills that can help a person to adapt and compensate for severe damage.
Physical Therapy

Physical therapy is designed to improve a person's strength, gross coordination, and balance. This type of rehabilitation helps people, after their stroke, regain their ability to walk and do other things like using stairs or getting out of a chair. Regaining fine motor skills like buttoning a shirt or using a knife and fork or writing a letter are activities that occupational therapy is designed to aid.
Stroke Recovery: Talk Therapy

Some people have problems coping with their new disabilities after a stroke. It is common for people to have emotional reactions after a stroke. A psychologist or other mental health professional can help people adjust to their new challenges and situations. These professionals use talk therapy and other methods to help people with reactions such as depression, fear, worries, grief, and anger.
Preventing Another Stroke: Lifestyle

The methods previously discussed that may prevent or decrease a person’s stroke risk are essentially the same for people who have had a stroke (or TIA) and want to prevent or decrease their chances of having another stroke. In summary, quit smoking, exercise, and if obese, lose weight. Limit alcohol, salt, and fat intake and get into the habit of eating more vegetables, fruits, whole grains, and more fish and less meat.
Prescribed Medications and Side Effects

Medications are usually prescribed for people with a high risk of stroke. The medicines are designed to lower risk by inhibiting clot formation (aspirin, warfarin and/or other antiplatelet medicines). Also, antihypertensive medications can help by reducing high blood pressure. Medications have side effects, so discuss these with you doctor.
Preventing Another Stroke: Surgery
There are some surgical options for stroke prevention. Some patients have plaque- narrowed carotid arteries. The plaque can participate in clot formation in the artery and can even shed clots to other areas in the brain’s blood vessels. Carotid endarterectomy is a surgical procedure in which the surgeon removes plaque from the inside of the arteries to reduce the chance of strokes in the future.
Preventing Another Stroke: Balloon and Stent
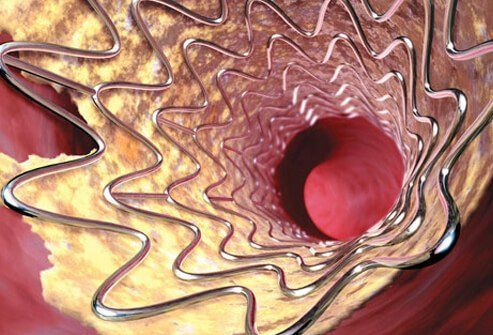
Some doctors also treat plaque-narrowed carotid (and occasionally other brain arteries) with a balloon on the end of a narrow catheter. Inflating the balloon pushes plaque aside and increases the vessel’s lumen (opens up the vessel). This opened artery then is reinforced (kept open) by an expandable stent that, when expanded, becomes rigid.
Life After a Stroke

About two-thirds of people (over 700,000) that have a stroke each year survive and usually need some level of rehabilitation. Some who get clot-busting drugs may recover completely, others will not. Many people who have disability after a stroke can function independently with therapy and rehabilitation methods. Although the risk of having a second stroke is higher after the first stroke, individuals can take the steps outlined in previous slides to reduce this risk.











